ONET FOR ALL OF YOUR CLAIMS MANAGEMENT
The Trusted Billing Partner Your Practice Needs- From office intake to billing, appeals and arbitrations, oNet Systems is a professional full-service out-of-network billing company.
- Whether elective, emergency or urgent procedures, oNet’s arsenal includes a firm grasp of insurance regulations, health plan policies and second-level processes to maximize out-of-network receivables for our clients.
- oNet’s team is skilled and experienced at overcoming the impediments that insurance companies construct to prevent providers from collecting prompt and fair payment for their services.
In-Office Consulting Services
oNet’s billing professionals will work with your staff to ensure a smooth claims process that begins before a patient is seen. We will review your staff manuals and documentation to ensure that you are communicating out-of-network policies clearly, concisely and in compliance with all regulatory edicts.
oNet’s best practices model includes comprehensive intake paperwork upon your first visit with a patient to ensure the myriad of out-of-network claim requirements are satisfied. We review your existing documentation and procedures to either replace, amend or fold-in what is missing to ensure the optimization of your out-of-network claims processing and management. Beyond standard demographics and privacy notice disclosures, we understand and implement the specific out-of-network processes needed to effectively challenge denials and/or sub-par reimbursements.


Physician Billing
Insurance companies are counting on your practice or agency to take a misstep or to simply give up on trying to reverse a claim’s nonpayment or underpayment. They understand that provider groups, facilities and government agencies have staff limitations and, as such, the longer a claim lingers, the more likely statutory limitations – as well as office resources – will be exhausted and a claim written off. With oNet on your side, you can maximize your receivables through the use of a better and more comprehensive claims management system – the oNet System. There are two key components to successful out-of-network billing and oNet excels at both. The first is claim submissions. Our experienced team understands the necessity of comprehensive pre-authorizations and accurate coding/pricing, as well as the nuances of effective and timely filing. The second, but equally important, component is the post-submission claims process. Critical to revenue maximization is having the combined knowledge and persistence to negotiate geographically-specific fair levels of reimbursement and to pursue all available means of claim resolution with payors.
Full-Spectrum Medical Debt Collections
oNet maintains an integrated medical debt collection partnership with a company that is licensed and insured to perform third-party collections. Systems of assignment can be customized from automatic to case-specific with run plans that vary by client and type of account. From soft billing within oNet to classic agency collections (e.g., comprehensive skip tracing, dunning, credit reporting, legal action and judgment enforcement), our platform is designed to seamlessly integrate what is needed, required and desired to efficiently and effectively complete the billing and claims management processing cycle.
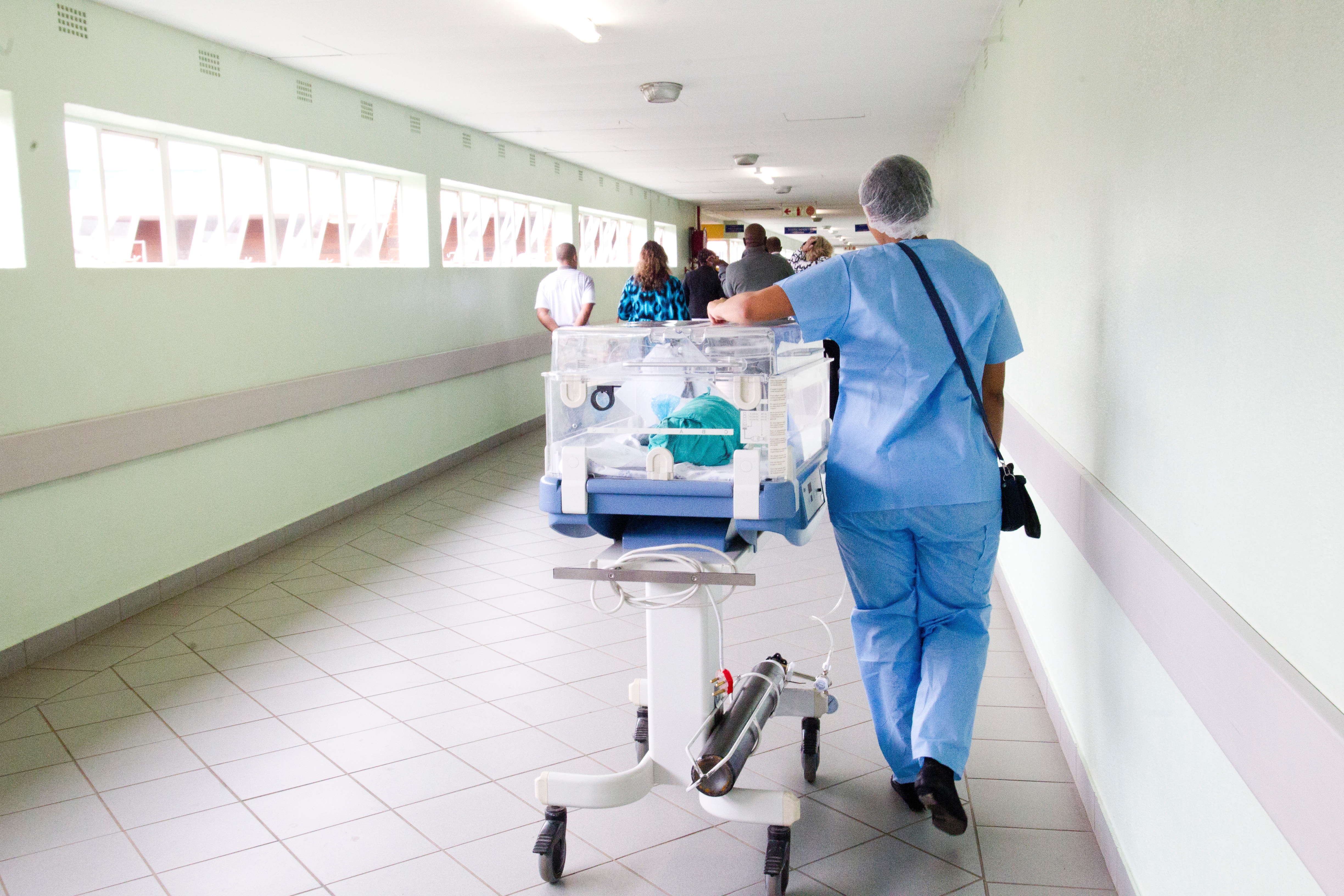
Emergency and Surprise Bill Law Arbitrations
oNet was founded and is principally located in New York State. The importance of this fact correlates to March 31, 2015, which is the date New York State’s Emergency Medical Services and Surprise Bills Law went into effect. This New York State “surprise bills” law was the first of its kind in the nation and has become the model for a growing number of other States’ enactment of their own version of the law. oNet’s team has been navigating and filing dispute resolutions under the original New York law since its inception and continues to remain ahead of the regulatory curve.
Ambulance and EMS Billing
Ambulance and EMS billing is not simply a straight-forward claims paradigm. Whether an emergency ambulance bureau, a municipality, an ALS first response group or a private ambulance service, oNet understands that the EMS revenue cycle requires additional billing elements, including electronic and paper claim submission, HIPAA-compliant data sharing, government, commercial and private billing, PCR review and compliant utilization, red-flag identity theft protocols, customized A/R reporting and collections, appropriate application and, as needed, creation of financial assistance policies, and integrated No-Fault and Workers’ Compensation billing and denial follow up.


Emergency Claims Recovery
oNet’s depth of knowledge when it comes to emergency services billing and regulatory frameworks dovetails with its unique ability to work with out-of-network providers to audit and collect upon past emergency services claims that previously went unpaid or underpaid. This category would cover out-of-network claims for (a) services performed in an Emergency Room; (b) services performed on an emergent or urgent basis; or (c) inpatient procedures rendered for patients admitted through a hospital’s emergency department. For these providers, oNet can work cooperatively with a practice’s existing billing team to analyze and collect upon older claims that we feel did not pay in accordance with acceptable reimbursement standards.
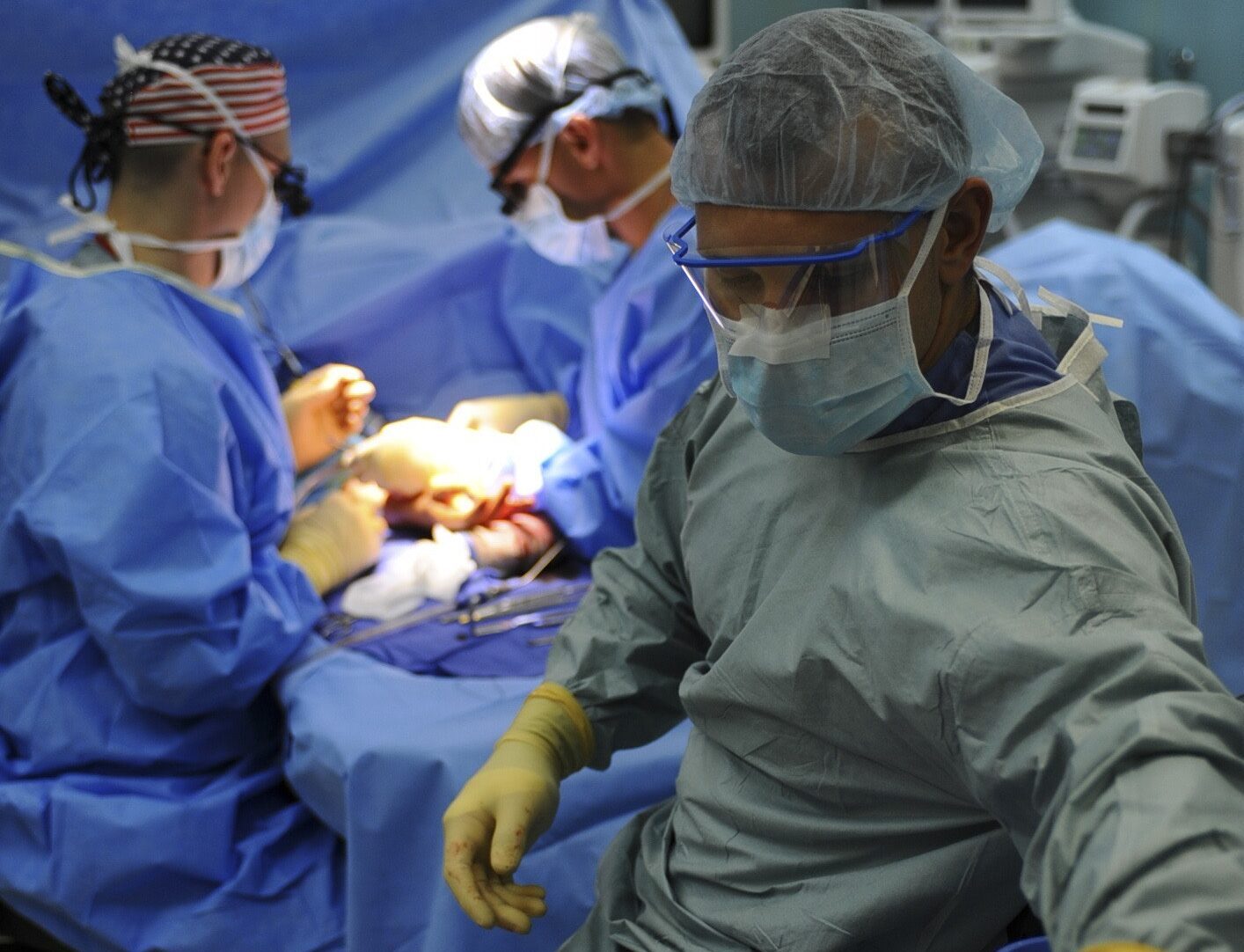
Facility Billing
oNet has a unique grasp of facility billing that combines regulatory compliance with smart revenue strategies. Facilities need a comprehensive system of pre-surgical and post-procedure workflow to diminish denials caused by a variety of shortfalls, including pre-authorization errors on the rendering provider side and incomplete claims management follow-up with the various payors. Facilities also have the unique ability to shape, whether through the expansion or narrowing of, their offered services in order to maximize receivables. As part of our billing platform, oNet provides our facility-clients with the consulting and analytics necessary for them to make these informed business shifts.
Credentialing
For both our physicians and facilities, oNet’s credentialing department provides full-service dual-side and ongoing credentialing that can remove or add our clients to and from insurance networks in a targeted fashion.
